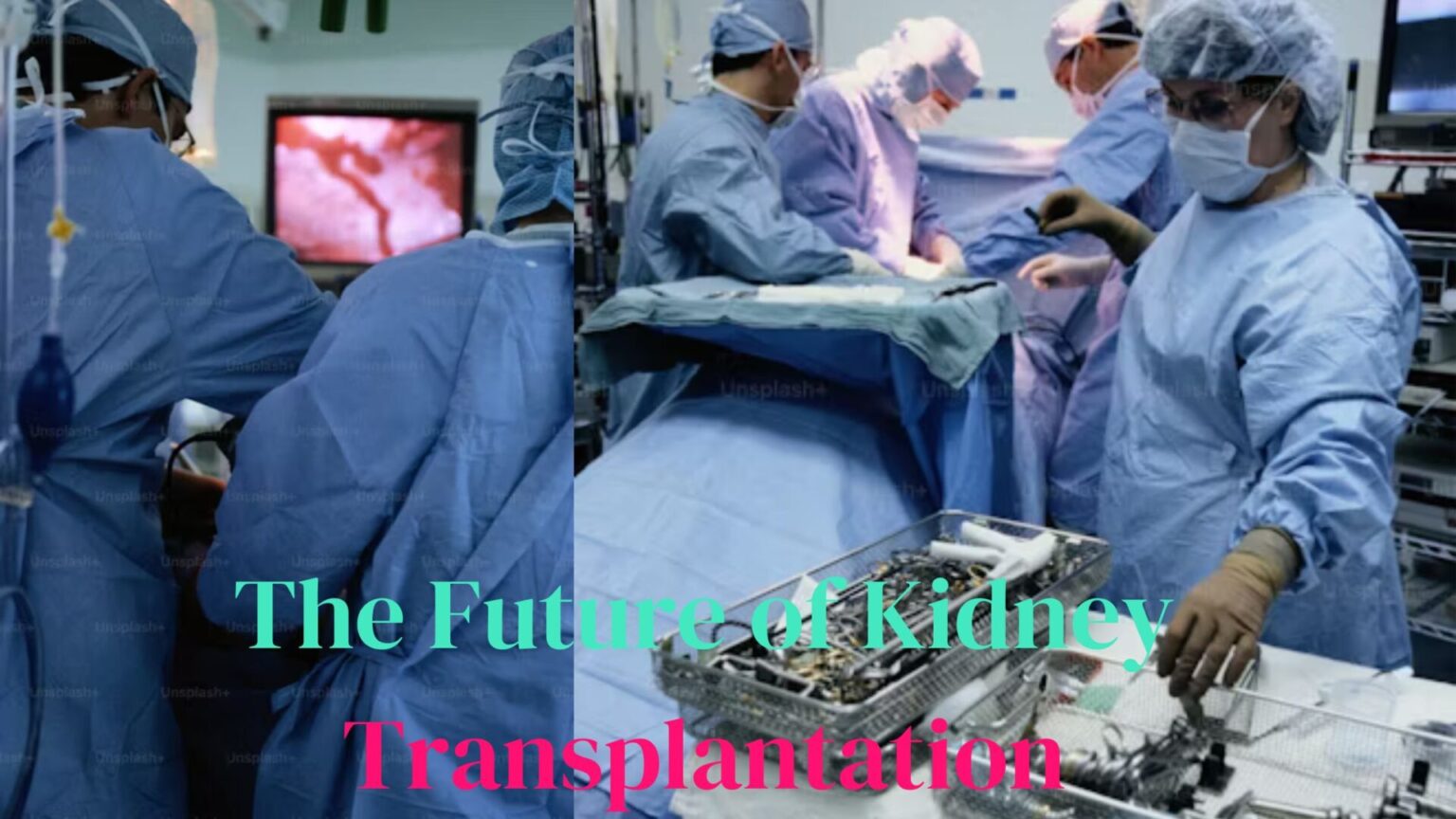
Introduction:-
Unlocking the Potential: The Future of Kidney Transplantation and Recovery
In recent years, advancements in medical science have revolutionized the landscape of kidney transplantation and recovery. With cutting-edge technologies and innovative approaches, researchers and healthcare professionals are continuously pushing the boundaries to enhance the success rates of kidney transplants and improve the quality of life for transplant recipients. In this article, we’ll delve into the promising developments shaping the future of kidney transplantation and recovery.
The future of kidney transplantation and recovery
- Precision Medicine: One of the most exciting prospects in kidney transplantation is the emergence of precision medicine. By leveraging genetic testing and molecular profiling, medical professionals can now tailor immunosuppressive therapies to individual patients, minimizing the risk of rejection and optimizing outcomes. This personalized approach holds immense promise for enhancing transplant success rates while reducing complications.
- Organ Preservation Techniques: Preservation of donor kidneys plays a crucial role in transplant success. Traditional methods involve cold storage, but novel techniques such as machine perfusion and normothermic preservation are gaining traction. These methods maintain the organ’s viability and function better, ultimately leading to improved graft survival and better patient outcomes.
- Regenerative Medicine: Regenerative medicine holds significant potential in revolutionizing kidney transplantation. Researchers are exploring various approaches, including stem cell therapy and tissue engineering, to regenerate damaged kidney tissues and improve organ function. These groundbreaking techniques offer hope for addressing the shortage of donor organs and improving long-term transplant outcomes.
- Artificial Intelligence (AI) in Transplantation: AI technologies are increasingly being integrated into various aspects of kidney transplantation, from donor matching to post-transplant monitoring. AI algorithms analyze vast amounts of data to predict patient outcomes, optimize organ allocation, and identify early signs of rejection. By harnessing the power of AI, healthcare providers can make more informed decisions, leading to better transplant outcomes and enhanced patient care.
- Enhanced Recovery Protocols: Improving the recovery process is essential for ensuring successful kidney transplantation. Enhanced recovery protocols focus on minimizing complications, reducing hospital stays, and promoting faster recovery post-surgery. These protocols incorporate strategies such as optimized pain management, early mobilization, and nutrition support, enabling transplant recipients to regain their health and functionality more rapidly.
- Telemedicine and Remote Monitoring: The adoption of telemedicine and remote monitoring technologies has transformed post-transplant care. Transplant recipients can now receive timely medical attention and support from the comfort of their homes, reducing the need for frequent hospital visits. Remote monitoring allows healthcare providers to track patients’ progress, monitor vital signs, and intervene promptly in case of any complications, leading to better overall outcomes and improved patient satisfaction.
- Psychosocial Support Services: Comprehensive care extends beyond the medical aspects of kidney transplantation to encompass psychosocial support for patients and their families. Integrating counseling, support groups, and mental health services into transplant programs can address the emotional challenges associated with the transplant journey, enhance coping mechanisms, and improve overall well-being.
- Ethical Considerations and Policy Reform: As the field of kidney transplantation evolves, ethical considerations and policy reforms are essential for ensuring equitable access to transplant services and addressing disparities in healthcare. Efforts to promote organ donation, reduce waiting times, and enhance transplant equity are paramount to maximizing the benefits of advanced transplant technologies for all patients in need.
What role will artificial intelligence play in predicting transplant outcomes and optimizing organ allocation in the future of kidney transplantation?
Artificial intelligence (AI) is poised to revolutionize kidney transplantation by significantly enhancing the prediction of transplant outcomes and optimizing organ allocation processes. Here’s how AI can play a pivotal role in shaping the future of kidney transplantation:
- Predictive Analytics: AI algorithms can analyze vast amounts of patient data, including demographic information, medical history, genetic markers, and biomarkers, to predict the likelihood of transplant success or failure. By identifying patterns and correlations within these datasets, AI can generate more accurate prognostic models, enabling healthcare providers to make informed decisions about patient selection and treatment strategies.
- Risk Stratification: AI-powered risk stratification models can assess the probability of complications, such as rejection, infection, or graft failure, based on individual patient characteristics and clinical parameters. By stratifying patients into risk categories, healthcare providers can tailor interventions and monitoring protocols to mitigate potential risks and optimize post-transplant outcomes.
- Optimized Organ Allocation: AI algorithms can analyze donor characteristics, recipient profiles, and historical transplant data to optimize organ allocation processes. By considering factors such as donor-recipient compatibility, organ quality, ischemia time, and waitlist urgency, AI can identify the most suitable matches and allocate organs more efficiently, maximizing the chances of transplant success and minimizing waitlist times.
- Real-Time Decision Support: AI-based decision support systems can provide real-time guidance to transplant teams during organ offers and allocation decisions. By synthesizing relevant clinical information and predictive analytics, these systems can assist clinicians in weighing the risks and benefits of potential transplant opportunities, facilitating more informed and timely decision-making.
- Continuous Learning and Improvement: AI-powered systems have the capability to continuously learn from new data and outcomes, refining predictive models and decision algorithms over time. By iteratively analyzing outcomes and updating algorithms based on real-world feedback, AI can adapt to evolving trends and improve its accuracy and reliability in predicting transplant outcomes and optimizing organ allocation strategies.
- Resource Optimization: AI-driven optimization algorithms can help healthcare systems allocate resources more efficiently by forecasting transplant demand, optimizing transplant center workflows, and streamlining logistical processes. By optimizing resource allocation and utilization, AI can enhance the overall efficiency and sustainability of kidney transplantation programs, ensuring that transplant services are accessible to all patients in need.
How might regenerative medicine techniques, such as stem cell therapy and tissue engineering, revolutionize kidney transplantation by addressing the shortage of donor organs?
Regenerative medicine techniques, including stem cell therapy and tissue engineering, have the potential to revolutionize kidney transplantation by addressing the persistent shortage of donor organs. Here’s how these innovative approaches can contribute to overcoming the organ shortage crisis:
- Bioengineered Kidneys: Tissue engineering holds promise for creating bioengineered kidneys in the laboratory using a combination of stem cells, biomaterial scaffolds, and bioreactor systems. These bioengineered kidneys can be tailored to match the recipient’s specific needs, minimizing the risk of rejection and eliminating the need for donor organs. By producing an unlimited supply of functional kidneys, tissue engineering could alleviate the dependency on donor organs and significantly reduce transplant waiting times.
- Stem Cell Therapy: Stem cells, with their unique ability to differentiate into various cell types, offer potential therapeutic applications for kidney regeneration and repair. Mesenchymal stem cells (MSCs), in particular, have been investigated for their immunomodulatory and regenerative properties in preclinical and clinical studies. By administering MSCs or other stem cell populations directly into the kidney or systemic circulation, researchers aim to promote tissue regeneration, reduce inflammation, and improve kidney function in patients with chronic kidney disease (CKD) or acute kidney injury (AKI).
- Organ Decellularization and Recellularization: Another approach involves decellularizing donor kidneys to remove cellular components while preserving the extracellular matrix (ECM) architecture. The decellularized scaffolds can then be repopulated with patient-derived cells, such as induced pluripotent stem cells (iPSCs) or renal progenitor cells, to regenerate functional kidney tissue. This process, known as organ recellularization, offers a potential solution for creating personalized, immunocompatible kidneys for transplantation, bypassing the limitations of donor organ availability.
- Xenotransplantation: Xenotransplantation involves transplanting organs or cells from non-human sources, such as pigs, into human recipients. Recent advancements in genetic engineering, including the development of gene-edited pigs with reduced immunogenicity and enhanced compatibility with the human immune system, have renewed interest in xenotransplantation as a potential solution to the organ shortage. By harnessing the regenerative capacity of xenogeneic organs and cells, researchers aim to overcome the limitations of human donor availability and provide lifesaving treatment options for patients in need of kidney transplantation.
- Cell-Based Therapies for Regenerative Medicine: Beyond stem cell therapy, emerging cell-based therapies, such as renal progenitor cells, kidney organoids, and renal tubular epithelial cells, offer additional avenues for kidney regeneration and repair. These cell-based approaches aim to replenish damaged or dysfunctional renal cells, restore tissue integrity, and promote functional recovery in patients with kidney disease or injury. By harnessing the regenerative potential of these cells, researchers seek to develop novel treatments for kidney disorders and reduce the reliance on donor organs for transplantation.
How will advancements in nanotechnology enable targeted drug delivery systems to minimize the side effects of immunosuppressive medications and enhance patient compliance in kidney transplant recipients?
Advancements in nanotechnology offer promising solutions to enhance the effectiveness of immunosuppressive medications while minimizing side effects and improving patient compliance in kidney transplant recipients. Here’s how nanotechnology-enabled targeted drug delivery systems can revolutionize post-transplant care:
- Precision Drug Delivery: Nanotechnology allows for the precise targeting of immunosuppressive drugs to specific cells or tissues involved in the immune response. By encapsulating these medications within nanocarriers, such as liposomes, nanoparticles, or dendrimers, drug delivery can be controlled and targeted to the site of action, such as the transplanted kidney or immune cells. This targeted approach minimizes systemic exposure to the medication, reducing off-target effects and enhancing therapeutic efficacy.
- Prolonged Drug Release: Nanotechnology enables the sustained release of immunosuppressive drugs over an extended period, ensuring a continuous and controlled supply of medication to maintain therapeutic levels. By modulating the properties of nanocarriers, such as particle size, surface charge, and composition, drug release kinetics can be tailored to match the patient’s specific dosing requirements. Prolonged drug release minimizes the need for frequent dosing, simplifying the treatment regimen and improving patient compliance.
- Enhanced Bioavailability: Nanotechnology-based drug delivery systems can improve the bioavailability of immunosuppressive medications by enhancing their solubility, stability, and cellular uptake. By encapsulating hydrophobic drugs within hydrophilic nanocarriers or incorporating drug-polymer conjugates, nanotechnology overcomes the limitations of poor drug solubility and bioavailability, ensuring optimal drug delivery and therapeutic efficacy.
- Reduced Side Effects: Targeted drug delivery to the site of action minimizes systemic exposure to immunosuppressive medications, reducing the risk of systemic side effects such as nephrotoxicity, gastrointestinal disturbances, and metabolic complications. By sparing healthy tissues from exposure to high drug concentrations, nanotechnology-based delivery systems mitigate off-target effects and enhance the safety profile of immunosuppressive therapy, improving patient tolerance and acceptance of treatment.
- Personalized Medicine: Nanotechnology enables the customization of drug delivery systems based on individual patient characteristics, such as pharmacogenomics, disease status, and comorbidities. By tailoring nanocarriers to match the patient’s specific needs, healthcare providers can optimize treatment outcomes and minimize adverse reactions, fostering a personalized approach to post-transplant care.
- Multifunctional Nanocarriers: Beyond drug delivery, nanotechnology offers opportunities to develop multifunctional nanocarriers capable of performing additional therapeutic functions, such as imaging, diagnostics, and targeted therapy. By incorporating imaging agents or therapeutic payloads into nanocarriers, clinicians can monitor drug distribution in real-time, assess treatment response, and adjust therapy accordingly, maximizing the effectiveness of immunosuppressive treatment in kidney transplant recipients.
Conclusion
In conclusion, the future of kidney transplantation and recovery is filled with promise, thanks to ongoing research, technological innovations, and advancements in patient care. By embracing emerging technologies, personalized approaches, and holistic care models, we can usher in a new era of transplant medicine where every patient has the opportunity for a successful transplant and a better quality of life.